Welcome
Cirillo Institute
Bryn Mawr Skin & Cancer Institute, Cirillo Cosmetic Dermatology Spa, and the Cirillo Center for Plastic Surgery work together to offer our patients the most comprehensive dermatology and plastic surgery center in Bryn Mawr, Newtown Square, and all of Philadelphia and the Tri-State area.

Members can earn
Double Points on
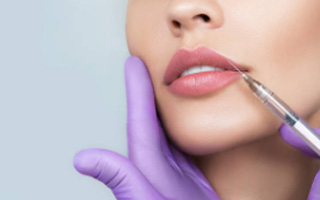
BOTOX®
one $50 BOTOX®
Cosmetic Gift Card
and get one free
DERMATOLOGISTS & PLASTIC SURGEON
DERMATOLOGISTS & PLASTIC SURGEON

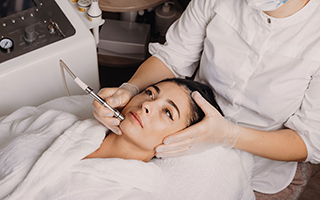
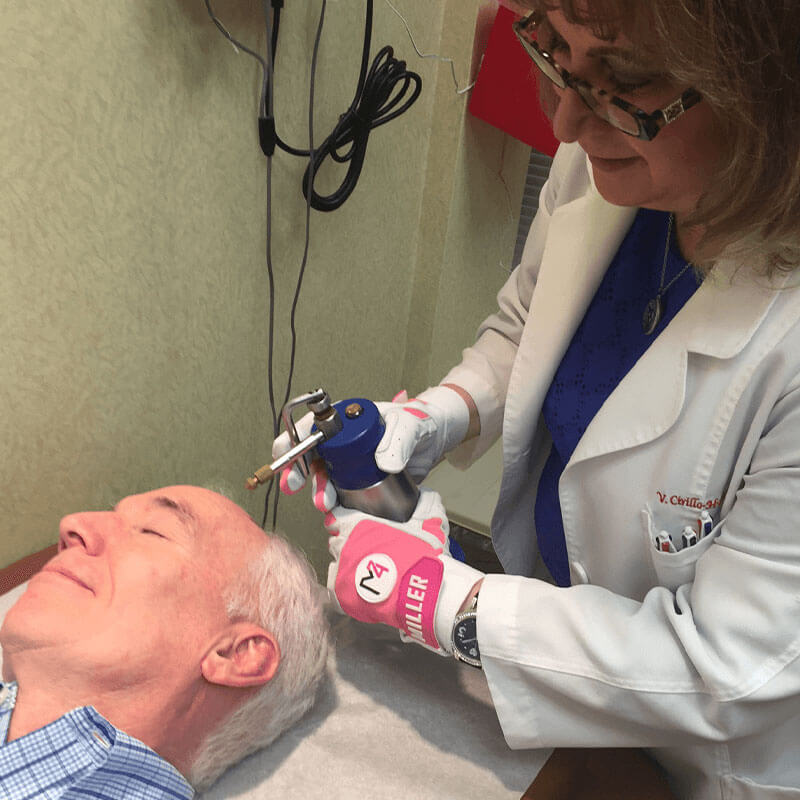
Our Services

Patient Testimonials
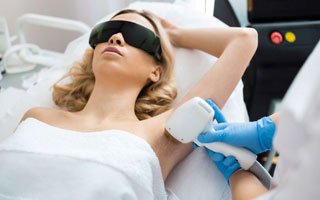
Each time I go to Cirillo Cosmetic Dermatology Spa I walk in there with confidence and peace of mind because I am always taken care of by the best staff of people there. They make sure that I am comfortable and pleased before I walk out the door.
I am very pleased😊 –D.G.
(Google Reviews, Cirillo Cosmetic Dermatology Spa, January 2022)
Very professional, as well as welcoming and a relaxed environment. The staff are all lovely people. Lisa is just the best at what she does and she is just simply a wonderful person. I could not ask for any better then what I experience at every visit at Cirillo. –C.K.
(Google Reviews, Cirillo Cosmetic Dermatology Spa, November 2021)
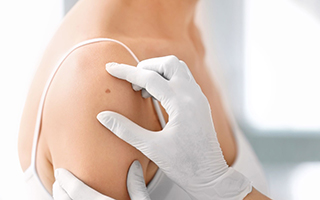
I was nervous going in for Mohs Surgery this morning but as soon as I got there the staff put me at ease! Everyone was very personable and professional. I would recommend this place to everyone! Dr was awesome! –C.T.
(Google Reviews, Bryn Mawr Skin & Cancer Institute, January 2022)
The office staff are always helpful and friendly. And Dr Heidary is top notch! She is thorough and knowledgeable and takes her time. She makes you feel like a person – not just a patient! –B.A.
(Google Reviews, Bryn Mawr Skin & Cancer Institute, January 2022)
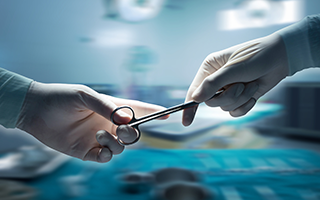
Dr. Gowan and the entire staff are nothing short of amazing. When making calls to multiple plastic surgeons, something never sat right with me. The first time I called Dr. Gowan’s office, I knew I found my doctor before even having my consultation, and it started with the office staff. The work, care and attention Dr. Gowan did for me was absolutely outstanding. Just one month out from my breast reduction, I feel like a new person and can still depend on Dr. Gowan to field any and all questions. –L.M.
(Google Reviews, Cirillo Center For Plastic Surgery, October 2021)
Two Convenient Locations
Newtown Square Office
CONTACT CIRILLO INSTITUTE
What is your Reason for Visit? How can we help you achieve your goals?

-updt.png)